Mpox (Monkeypox)
Information and resources regarding the mpox virus.
Mpox Vaccine Sites
Mpox Vaccine Sites
For People with Confirmed Mpox by Testing
In May 2022, mpox was identified in the United States in a Massachusetts resident who traveled outside the country. Since then, mpox has been identified in every state in the U.S. and in more than 100 countries where cases do not typically occur.
Mpox is rare and does not spread easily between people without close contact. The threat of mpox to the general U.S. population remains LOW.
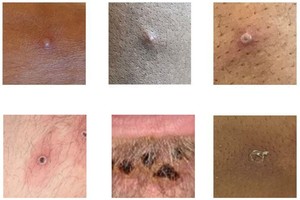
Photo courtesy: UK Health Security Agency (UKHSA)
Symptoms are most often mild, but in rare cases a more severe illness can occur that might require hospitalization. See below resources and FAQs for more information.
Digital Resources
Press Releases
- NH DPHS Updates Mpox Vaccine Eligibility (September 26, 2022)
- First Pediatric Case of Mpox Identified in New Hampshire (September 16, 2022)
- NH DPHS Expands Mpox Vaccine Eligibility, Vaccination Locations (August 29, 2022)
- First Probable Case of Mpox Identified in New Hampshire (June 29, 2022)
How can people with mpox reduce spreading mpox to others?
Anyone with mpox should:
- Stay home and away from other people and animals, including people and animals in the home,
- Stay in their own room and use their own bathroom,
- Limit touching commonly used objects,
- Avoid sharing objects (towels, washcloths or drinking from the same glass),
- Clean and disinfect touched surfaces other people may come into contact with,
- Be careful how clothes and linens are washed/cleaned,
- Cover furniture or other items that cannot be washed,
- Wash hands often or use an alcohol-based hand sanitizer,
- Avoid touching the rash; keep skin rash and sores covered, (do not shave, pop or scratch the sores),
- Wear a well-fitting mask, if contact with others cannot be avoided, such as, going to the doctor's office or when around others in the home.
Use the above tools until the scabs have fallen off and a new layer of skin has formed.
It is also important for people living in the same house with a person who has mpox to wear a well-fitting mask to protect themselves. Especially if helping them with personal or medical care.
Go to the CDC for further details and instructions.
If I have mpox, how long do I need to isolate?
People with mpox should isolate at home until all scabs have fallen off and a fresh layer of intact skin has formed.
This could take up to 2-4 weeks from the time symptoms start.
If a person with mpox cannot isolate completely while sick, take precautions to limit the chance of spreading mpox to others.
- Wear a well-fitting mask and cover lesions while around others.
- Disinfect/Clean surfaces in shared bathrooms or rooms between each use.
- Avoid sharing objects (e.g., towels, washcloths, drinking from the same glass).
- Cover upholstered furniture and porous materials that cannot be washed.
I was diagnosed with mpox, but am nervous to tell my partner(s).
You can tell your partners anonymously using the Tell Your Partner website: https://tellyourpartner.org
I was diagnosed with mpox. What should I do about caring for my pet?
Although there have been no reports of pets becoming sick with mpox in the United States, it is still recommended people with mpox limit contact with animals, especially rodents and lagomorphs (hares, rabbits), until more information is known about the virus (including the spreading of the virus) in the United States.
- When possible, another person should care for the pet.
- The person with mpox should avoid contact with the pet, including petting, snuggling, being kissed or licked, and sharing food.
- If a person with mpox must care for the pet while they are sick, they should wear long sleeves, disposable gloves, and a face covering as well as washing hands before and after interacting with them. Making sure to cover the rashes or skin sores related to the mpox virus should be done to limit the pet’s contact with virus.
Follow these tips until you fully recover and disinfect (sanitize/clean) your home before bringing your pet(s) back to the home.
More information about care for pets in the home people with mpox can be found at the webpage: Mpox in Animals and Pets (CDC).
Cleaning & Disinfection
How should people with mpox clean and disinfect their home?
The CDC provides general guidance on cleaning and disinfecting the home. Please review the guidance at https://www.cdc.gov/poxvirus/mpox/if-sick/cleaning-disinfecting.html.
Are there any special instructions for how to wash clothing and linens that have been in contact with an mpox rash?
People with mpox should handle their own laundry and keep it separate from the laundry of the other people in the home. Soiled laundry should never be shaken or handled in a way that could spread infectious particles. Laundry should be kept in an impermeable container that can be disinfected after, or in a fabric bag that can be washed with the clothing. Landry can be washed in a standard washing machine with regular detergent (follow label instructions). Avoid public laundry facilities.
See CDC’s guidance for more details: https://www.cdc.gov/poxvirus/mpox/if-sick/cleaning-disinfecting.html
Go to State-by-State Case Counts (CDC)
Hover over New Hampshire for the number of cases or scroll down to the bottom of the page for a downloadable Excel file.
Healthcare Provider Resources
CDC Resources
Resources for Residents
Resources for Schools/Childcare
For People with Possible Exposure to Mpox
I think I was exposed to mpox - what should I do?
Call your healthcare provider right away and let them know you think you were exposed to mpox. Based on your situation, your healthcare provider can help determine if you might benefit from being given the JYNNEOS vaccine, which can help prevent infection if given early after an exposure. If you do not have a primary health care provider, please call 603-271-4496.
How soon after exposure to Mpox do symptoms appear?
If you have been exposed to someone with Mpox, symptoms will usually occur 7-14 days after exposure, but can range from 5-21 days.
If I have a rash or other symptoms suspicious for Mpox after exposure, what should I do?
Call your healthcare provider right away and let them know about your symptoms and potential exposure to someone with Mpox. Your healthcare provider will arrange for testing. You should isolate yourself from others until you know the results of the test. If you do not have a healthcare provider, please call 603-271-4496.
Vaccine Questions (Pre-Exposure Prophylaxis and Post-Exposure Prophylaxis)
Is there a vaccine to prevent mpox?
Yes. The JYNNEOS vaccine is the only FDA-approved vaccine to prevent mpox and is given as a 2-dose series. The second dose is given 28 days after the first dose. People have maximal protection starting about 14 days after the second dose. Those who are vaccinated should still take precautions to avoid infection since the vaccine does not provide 100% protection (see recommendations above for preventing mpox). Even if vaccinated, people should avoid close or physical contact with someone who has mpox.
How effective is the JYNNEOS™ vaccine?
The JYNNEOS vaccine is effective at reducing the risk of mpox. Two doses of the JYNNEOS vaccine are recommended to provide the most protection. Data from the mpox outbreak in the U.S. last year show 2 doses of the JYNNEOS vaccine were 69% effective at preventing mpox, while getting only one dose was 37% effective. For more information, visit CDC's web page about the effectiveness of the JYNNEOS vaccine.
Is the JYNNEOS™ vaccine safe in patients who are pregnant or breastfeeding?
There is not much human data on use of the vaccine in people who are pregnant, but animal studies have shown no evidence of harm to a developing fetus. Similarly, the vaccine has not been studied in people who are breastfeeding or in young children. JYNNEOS can be offered to people who are pregnant or breastfeeding who are otherwise eligible. Please discuss with your healthcare provider the risks and benefits of JYNNEOS.
Who is eligible to get the JYNNEOS™ vaccine in NH?
To receive a vaccine, in New Hampshire, you must:
- Live in NH
- Work in NH, or
- Have a primary care healthcare provider in NH
NH DPHS recommends you receive the JYNNEOS vaccine if you:
- Know you have been exposed to the mpox virus in the last 14 days, or
- May be more likely to get the mpox infection (BEFORE being exposed to the virus), including men who have sex with men who reported:
- Having three (3) or more new sex partners in the last month,
- Engaging in group or anonymous sex,
- Having sex at sex-on-site venues/events,
- Taking medicine to prevent HIV (HIV PrEP).
NH DHHS will post updates on vaccine eligibility on mpox webpage.
Where can I get the Mpox vaccine?
Because the JYNNEOS vaccine supply continues to be limited, persons seeking to get the vaccine will require an appointment.
- IF you HAVE a primary care provider, call your provider and ask if the vaccine is right for you.
If yes, ask your provider to make a referral to one of the listed clinic sites to schedule an appointment.
- IF you DO NOT HAVE a primary care provider, call one of the listed clinics on the website.
Can teens or children get the vaccine if they have been exposed to Mpox?
Yes. Under the FDA’s Emergency Use Authorization (EUA), people younger than 18 years of age, at risk of getting Mpox can be vaccinated. The JYNNEOS™ vaccine when given to children and adolescents is a subcutaneous injection (beneath the skin) in the upper arm.
Why are the FDA and CDC now recommending that the JYNNEOS vaccine be given in a different way?
Mpox virus infections continue to increase, and the number of vaccine doses that we have continue to be limited. To increase the number of people that can be vaccinated, the FDA and CDC are now recommending that adults 18 years of age or older who are at high risk for being exposed to the mpox virus be vaccinated with a lower dose of the JYNNEOS vaccine that is given between the top and bottom layers of skin on a person's forearm (called an "intradermal" injection). When the vaccine is given in this way, it has been shown to produce the same level of antibody protection compared to a higher dose of the same vaccine given beneath the skin layers (called a "subcutaneous" injection). Administering the vaccine between the skin layers (intradermally) can only be given in this way for adults 18 years of age or older, and it is an important way to increase the number of people who can be vaccinated (because of the lower dose used) while still offering a high-level of protection. Children and adolescents who may need to be vaccinated can also be vaccinated with the same JYNNEOS vaccine, but for people under the age of 18 years, the vaccine will still be given at the standard dose given beneath the skin (subcutaneously).
The vaccine is safe when it is given both ways, but people given the vaccine between skin layers (intradermally) may be more likely to develop local reactions, like redness, swelling, itching, or discomfort at the injection site. And those local reactions may last for a longer period of time.
Treatments
What treatments are available for Mpox?
Most Mpox illnesses are mild and resolve on their own without treatment. However, for people who develop more severe disease, or who are at high risk of developing severe disease (such as people with weakened immune systems and pregnant people), Tecovirimat® (TPOXX) may be recommended. Talk to your doctor to see if treatment is right for you.
Have additional questions? Call 603-271-4496 (after hours call 603-271-5300). For vaccine questions, call 603-271-4482.



